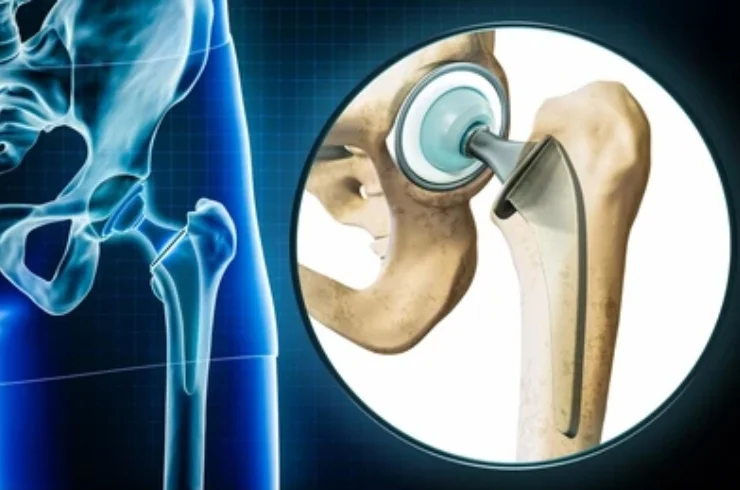
Hip Replacement: A Comprehensive Guide
Hip replacement surgery, or hip arthroplasty, involves removing a damaged hip joint and replacing it with an artificial joint (prosthesis). It is typically performed to relieve pain and improve function in individuals with severe hip joint damage due to conditions like osteoarthritis, rheumatoid arthritis, or fractures.
The procedure includes a pre-operative assessment, induction of anesthesia, and surgical implantation of the prosthesis. Recovery involves hospital stay, pain management, and physical therapy to regain mobility. Potential risks include infection, blood clots, and implant loosening. Long-term management includes maintaining a healthy weight, engaging in low-impact exercise, and attending regular follow-ups to monitor joint health.